Corneal transplantation is the most common form of transplantation surgery occurring in the world and, globally, it provides improved vision to many thousands of people each year. NHMRC-funded researchers at Flinders Medical Centre and Flinders University have made major contributions to improving clinical and eye bank practice both in Australia and internationally, through their establishment of the Australian Corneal Graft Registry (ACGR), the largest registry of its type in the world.
The cornea is a transparent layer of tissue, about half a millimetre thick and 10-12 mm in diameter, that sits over the iris, pupil and lens at the front of the eye. It plays a number of roles, including focusing the light that passes through, filtering out ultraviolet light, and protecting the more internal parts of the eye from abrasion and chemical damage. Because it plays this protective role, the cornea is itself prone to injury and damage. While the body possesses a number of mechanisms to heal and repair the cornea, when healing is unsuccessful, damage can lead to impaired vision and blindness. The idea of replacing a damaged cornea with a transplant from another eye (also called keratoplasty, or a corneal graft) dates back hundreds of years, however it was not until 1905 that the first successful human-to-human corneal transplant was performed.1
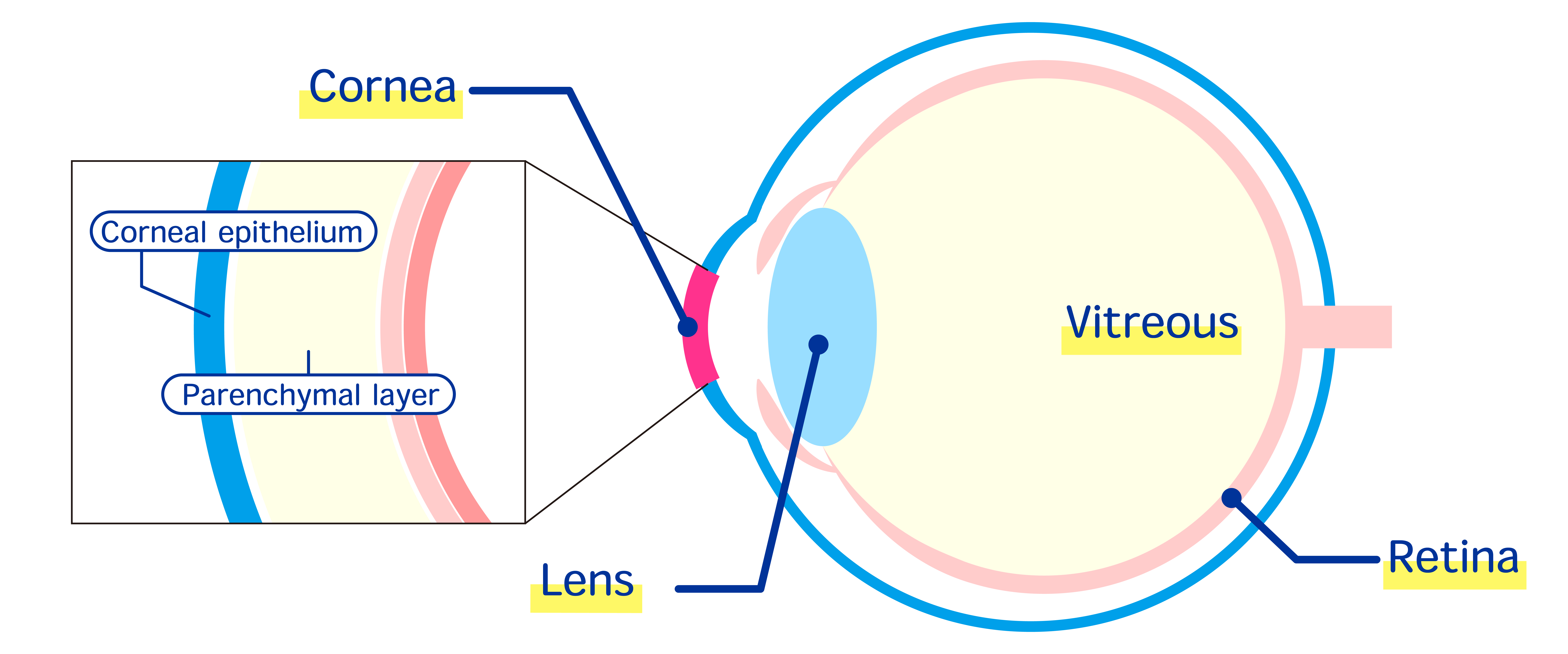
Following the establishment of corneal transplantation as a standard surgical procedure, the efforts of ophthalmic researchers began to be focused on improving success rates and eye bank practice. NHMRC-funded researchers would play key roles in revealing the factors that had the biggest impact on transplant success.
How are donor corneas for transplantation sourced?
Eye banks retrieve human eyes from people who have died, having gained consent from the next-of-kin. Once retrieved by eye bank staff, the cornea is removed, stored in a preservation solution, and later delivered to an ophthalmic surgeon. Occasionally, corneas are transported interstate by air freight to another eye bank. Surgeons then transplant these corneas, using a variety of techniques.
Australia has five eye banks, licenced by the Australian Government’s Therapeutic Goods Administration (TGA).
Investment
NHMRC commenced operations in 1937, and in that same year provided its first grant to support research into corneal transplants.2 The cornea was the first tissue to be transplanted successfully in Australia and the first corneal transplant in Australia was performed in 1940.
The development of corneal transplantation and eye banking are inextricably linked, and the first Australian eye bank was established in Brisbane in the late 1940s.3
In May 1954, The Premier of Victoria wrote to the Prime Minister, asking that NHMRC discuss the establishment of eye banks nationwide, including supporting legislation. The Council supported the proposal but considered that any such legislation should permit the collection and storing of other human tissues required for transplantation purposes. Later, after a March 1981 Australian Health Ministers' Conference (AHMC) discussed the need for a code of practice for deceased donors for transplant organs and tissues, this issue too was referred to NHMRC for action. NHMRC established a working party to prepare a code, which was provided to AHMC in late 1982. A revised version was produced in 1990. In 1996, NHMRC endorsed a replacement to the code, the Recommendations for the Donation of Cadaveric Organs and Tissues for Transplantation which had been developed by NHMRC’s National Health Advisory Committee.
NHMRC has provided a succession of grants to support corneal transplant research. These include Project Grants to Barry Collin at the University of Melbourne (1968-1973), and Doug Coster and Keryn Williams at Flinders University (1986-1994) to develop the ACGR, plus a succession of grants to Williams for research related to corneal disease and transplants.
Other sources of funding for the ACGR include:
- The Pank Ophthalmic Trust (1987-1988)
- ACCORD (1992)
- AHMC (1993-1998)
- Commonwealth Department of Health and Ageing (2002-2009)
- Australians Donate (2000-2001)
- Australian Organ and Tissue Authority (2009-10 to 2025).
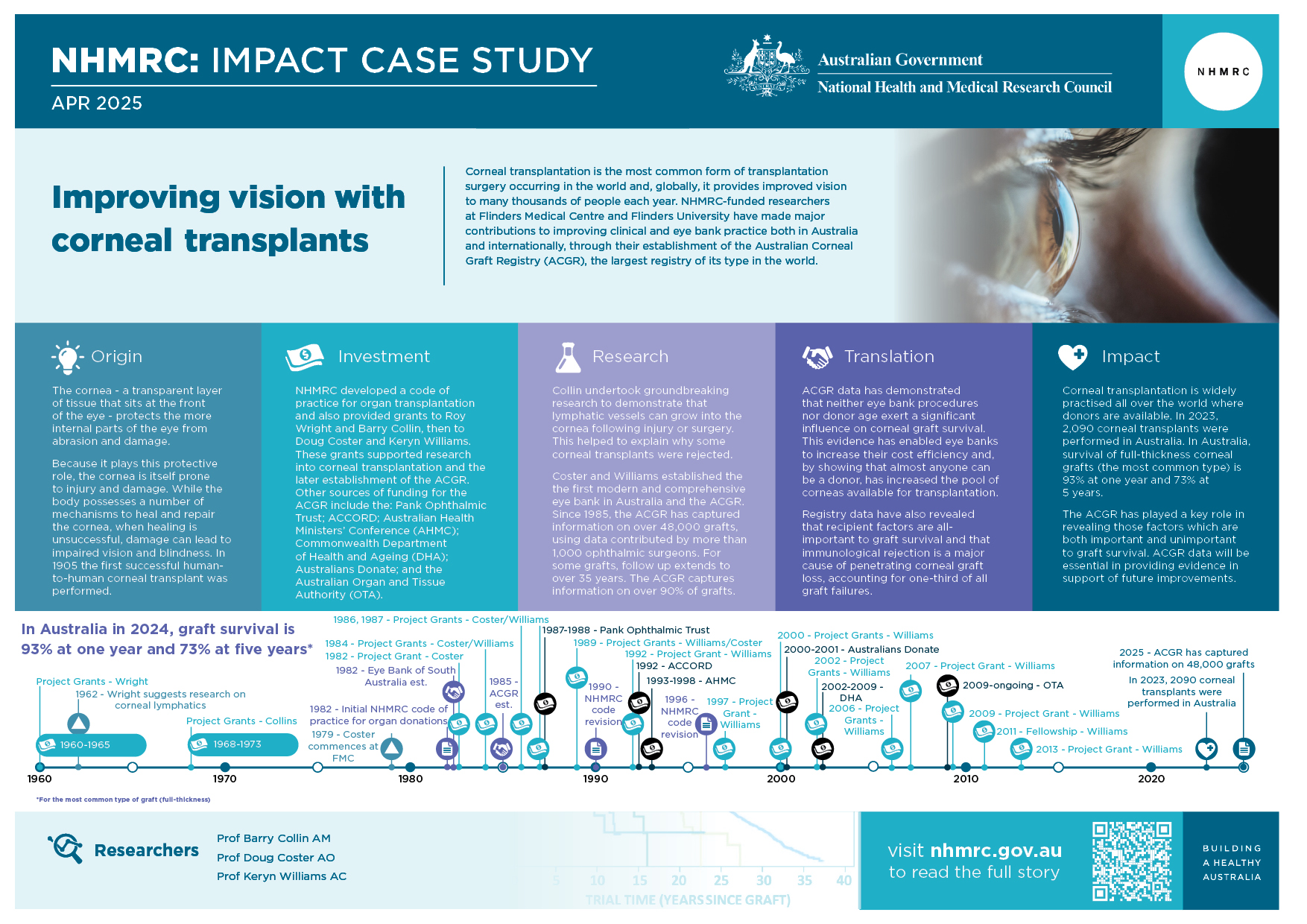
The PDF poster version of this case study includes a graphical timeline showing NHMRC grants provided and other events described in the case study.
Research
In 1962, Professor Roy Wright, Head of the NHMRC-funded Department of Physiology at the University of Melbourne, had an idea for a research project.
The cornea is normally devoid of blood and lymphatic vessels. This gives it an ‘immune privilege’, meaning that the immune system does not function there as it does elsewhere in the body. This in turn makes it possible to transplant a cornea from one person to another without the use of immunosuppressive drugs.
But Wright wondered whether lymphatic vessels might grow into the cornea following injury (or surgery). If they did, this might explain why some corneal grafts were rejected.
Wright approached Barry Collin, an optometrist with training in pathology, to investigate the question, and the results of Collin’s research were groundbreaking. They confirmed Wright’s idea and were published in a range of leading international journals during 1966.
While these findings challenged existing understanding within immunology, they conformed with the experience of ophthalmologists, who knew that corneal vascularisation was associated with unsuccessful transplants. Collin’s research over the next decade provided qualitative and quantitative descriptions of lymphatic growth and ways to prevent growth. This was important as it explained why and how the body can recognize the foreign tissue and improved options for treatment.
Collins’ work, undertaken in Australia, was the first major contribution that research had made internationally to improving the success of corneal transplantation, which up to that time had been predominantly a matter of clinical practice.
Inspired by this success, in 1979, when Doug Coster was appointed Director of Ophthalmology at the newly established Flinders Medical Centre in South Australia, he recognised that his first major task was to ensure that work at the Centre was research-based. He did this by recruiting immunologist Keryn Williams from Oxford University.
At Oxford, Williams’ research had been focused on kidney transplantation immunobiology and soon after her arrival in 1981, Williams and Coster established the Eye Bank of South Australia, the first modern and comprehensive eye bank in Australia.
From her experience at Oxford, Williams was closely acquainted with the power of comprehensive data collection for improving clinical outcomes. Consequently, the Flinders’ team’s next step, in 1985, was to establish – on the basis of the quality control system of the Eye Bank of South Australia and the records of surgeons working at Flinders Medical Centre – the Australian Corneal Graft Registry (ACGR).
The purpose of the ACGR was to undertake an ongoing census of all corneal grafts taking place in Australia, to improve data collection about corneal graft survival and failure and to quantify those factors affecting the outcome of corneal transplantation. The ACGR became, effectively, an ongoing prospective, longitudinal cohort study of corneal transplants performed across the country.
Following each procedure, surgeons would provide data to the Registry on a wide range of factors including details of the recipient, the donor, and the type of surgery performed. Subsequently, information on graft survival, visual outcome, and complications, interventions and significant events would be sought. Registration and follow-up would be entirely voluntary and there would be no charge to contributors.
The ACGR process described above has continued since the Registry’s inception, with the whole process overseen by an Advisory Board of senior contributing surgeons and approved by a Human Research Ethics Committee.
Translation
Since its commencement in 1985, the ACGR has captured information on over 48,000 grafts, using data contributed by more than 1,000 ophthalmic surgeons. For some grafts, follow up extends to over 35 years. The ACGR captures information on over 90% of grafts performed in Australia. Every five years, the ACGR is linked with the National Death Index to ensure that it includes information about when patients have died.
Ophthalmologists nation-wide, often working with scientists, have been enthusiastic about the value of the Registry since its inception. They have suggested questions that they wanted answered, co-designed the data collection forms and database structures, and continue to raise new questions and request regular database re-design as clinical practice has evolved.
Regular reports have been published based upon data collected within the Registry. The ACGR reports have been highly cited by researchers and have proven to be of great significance for corneal transplant surgeons, for the managers of eye banks, and for providing information on outcomes to patients. Analyses of the ACGR data are returned regularly to all contributors and eye banks and specific analyses are published in the international literature. Contributors are regularly provided with individualized outcome data and more detailed audits on request.
The ACGR has generated other benefits, including by providing information to eye banks to help with TGA registration, and to the Australian Government’s Medical Services Advisory Committee, to support continuation of a medical benefits schedule item related to corneal transplantation.
The Registry has been used as a model in several other countries when initiating their own corneal registries, and the extensive data held within the Registry is constantly being used in comparative studies globally.
Outcomes and impacts
Corneal transplantation is the most common form of transplantation undertaken in Australia,4 and the ACGR holds the largest collection of data on corneal transplantation in the world.
In Australia, survival of full-thickness corneal grafts (the most common type) is 93% at one year and 73% at 5 years. The ACGR has played a key role in revealing those factors which are both important and unimportant to graft survival. This in turn has enabled clinicians to more accurately predict which patients are most likely to have a successful transplant, and therefore to improve the experience of patients overall.
Before results from the Registry were first available, clinicians and researchers wondered whether graft survival was affected by donor factors and by the way that eye banks store corneas. However, data from the ACGR has demonstrated that neither eye bank procedures nor donor age exert a significant influence on corneal graft survival. The implication is that even quite elderly individuals - the oldest was 99 years old - can donate corneas for transplantation.
This type of evidence has increased the pool of corneas available for transplantation and has also enabled eye banks to concentrate their resources on areas of greatest need. It shows that almost anyone can be a donor and that, because donor corneas can safely be stored in the eye bank, surgery can be scheduled at a time convenient for the surgeon and patient.
Registry data have also revealed that recipient factors are all-important to graft survival. Over more than 30 years, factors such as a recipient’s age, sex, underlying health conditions and the state of their eye have repeatedly proved to be the most important discriminants of graft survival.
Further, immunological rejection has been found to be a major cause of penetrating corneal graft loss, accounting for one-third of all graft failures. As noted above, this finding has not been surprising to corneal surgeons but it has fundamentally challenged the concept of ‘immune-privileged’ sites within the body.
Corneal transplantation is widely practised all over the world where donors are available. In 2023, 2090 corneal transplants were performed in Australia5, compared with 953 in 20016. The success rate is high, at least in the short term, however, the long-term graft survival rate could be improved.
As eye banking and surgical techniques evolve, the impact of new developments on outcomes needs to be confirmed with evidence. The ACGR has been the major international contributor to this process and through the Registry, Australian corneal transplant surgeons have (to date) done more to evaluate the outcomes of their procedures than any other group of ophthalmic surgeons anywhere in the world.
Over the last 30–40 years, clinical transplantation in solid organ transplantation (i.e. kidneys, hearts, lungs and liver) has improved continuously, but this type of progress has not been seen with corneal transplantation. This is because the improvements in survival of solid organ grafts results mainly from improvements in immunosuppression and to a lesser extent, improved immunological matching. These two approaches are not broadly applicable to corneal transplantation. Alternative approaches to preventing rejection and enhancing engraftment for corneal transplants are required and need to be developed in the laboratory in the first instance. Use of ACGR data will be essential in providing evidence in support of these improvements.
Researchers
Professor Barry Collin AM
Hermann (Barry) Collin received a Bachelor of Science in Pathology (1956), a Master of Applied Science (1966) and Doctor of Philosophy in Physiology (1970), all at the University of Melbourne.
After being in optometric practice (1955—1961), Collin was a lecturer at the Victorian College of Optometry (1962—1974). He was also a Research Fellow in the physiology laboratory at the Sir William Dunn School of Pathology, Oxford University (1967—1968). He was then Reader, Department of Optometry, University of Melbourne (1973—1981) and a Fellow in the Department of Ophthalmology at the Harvard Medical School Eye Research Institute (1975).
Collin became Head of the School of Optometry at the University New South Wales (1982—1992) and then Professor of Optometry (1982—1994).
Collin’s contributions to optometry and medicine have been recognised in many ways. In 1991, Collin was elected to be a fellow, and the only optometrist fellow, of the Royal College of Pathologists, London. In 1997, Collin was appointed a Member in the Order of Australia to recognise his contributions to optometry and the science of medicine.
Professor Doug Coster AO
Douglas J Coster graduated in medicine from the University of Melbourne in 1969 and underwent postgraduate training in ophthalmology at the Royal Melbourne Hospital, the Royal Victorian Eye and Ear Hospital and subsequently at Moorfields Eye Hospital in London. In 1979, he was recruited back to Australia to become the Foundation professor of ophthalmology at the Flinders Medical Centre and Flinders University in Adelaide. Coster was co-founder of the Eye Bank of South Australia (1982).
Coster was appointed an Officer in the Order of Australia in 1991 and was awarded the Centenary Medal in 2001. He supervised accredited trainees in ophthalmology for over 20 years and mentored many corneal research fellows from all over the world.
Professor Keryn Williams AC
Keryn Anne Williams graduated from the University of Melbourne with a Bachelor of Science (1971), then after completing her doctoral research (1974) worked as a researcher at the University of Oxford with the Australian surgeon Peter Morris. Upon Morris’s recommendation, Doug Coster, recruited Williams to Flinders Medical Centre in 1981.
Williams was co-founder of the Eye Bank of South Australia (1982), founder of the ACGR (1985) and is currently its scientific director. Williams became Professor, School of Medicine, Flinders University of South Australia (2011) and in 2017 was appointed a Companion of the Order of Australia (AC) for eminent service to medical science in the field of ophthalmology.
Partner
This case study was developed with input from Professor Keryn Williams and Professor Doug Coster and in partnership with the ACGR at Flinders University.

References
The information and images from which impact case studies are produced may be obtained from a number of sources including our case study partner, NHMRC’s internal records and publicly available materials. Key sources of information consulted for this case study include:
1Moffatt SL, Cartwright VA, Stumpf TH. Centennial review of corneal transplantation. Clinical & experimental ophthalmology. 2005 Dec;33(6):642-57.
2 Research Grant to Dr Kevin J O'Day at St. Vincent's Hospital, Melbourne. Source: Commonwealth of Australia. Report of the National Health and Medical Research Council , Third Session, held at Sydney NSW, 12th and 13th November 1937.
3 Coster DJ. History of corneal transplantation in Australia. Clinical & experimental ophthalmology. 2015 Apr;43(3):268-76.
4 Mandel DT, Chapman JR. Transplantation in Australia—50 years of progress. Medical journal of Australia. 1992 Jul;157(1):46-50.
5 Data provided by ACGR
6 Keane MC, Coffey NE, Jones VJ, Lawson C, Mills RAD, Williams KA. The Australian Corneal Graft Registry, 2021/22 Adelaide, Australia, 2022. Report. Source: Australian Corneal Graft Registry Report 2021/22